5 great ways Physiotherapy can help manage Parkinson’s Disease

5 great ways Physiotherapy can help manage Parkinson’s Disease
Parkinson’s Disease
Parkinson’s Disease is a progressive degenerative disease of the brain that affects your ability to perform movements. As a result, people with Parkinson’s tend to have slow movements, resting tremors, stiffness, and poor balance. This is caused by the death of cells that produce the messenger dopamine. Dopamine is responsible for your movements and the ability to think and plan. Additionally, it is also responsible for producing feelings such as motivation and pleasure. This is why there are motor and non-motor symptoms associated with the disease. These changes in your ability to move can lead to an increased risk for falls which can lead to fractures, hospitalizations, or death, especially in older adults. Read on to find out how physiotherapy can help you manage Parkinson’s Disease!
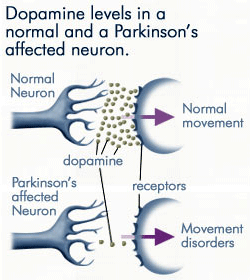
Presentation

People with Parkinson’s tend to have a typical appearance which includes a stooped posture, flexed limbs, masked face, resting tremors, and slow movements. Medications can also cause unwanted side effects such as uncontrollable movements and urges to move. In addition, people with Parkinson’s can have trouble producing movements which can cause problems with walking such as shuffling, freezing, faster, and smaller steps (festination). People with Parkinson’s disease can present in early, moderate, and late stages with a whole range of different limitations.
Parkinson’s Success Story
My first placement involved treating people with Parkinson’s disease virtually. One of the main concerns described by patients was the lack of information provided by their neurologists and doctors. Apart from medications, most people are unsure of how else they can manage their symptoms. Physiotherapists have a wealth of knowledge on ways to manage Parkinson’s Disease by improving your balance, strength, walking, health, and quality of life.
It was awesome to have knowledgeable people helping out with so many areas. A diagnosis of PD doesn’t come with a set of instructions. I learned more from this program than I did from my neurologist. Having a team helping me out felt like a support that I haven’t found with the medical community. It can be lonely living with a disease and this program helped with that. Thank you
How is Parkinson’s Disease managed?
Parkinson’s disease currently has no cure and is mainly managed by medications. These are used to bring down symptoms and help you get back to your daily activities rather than stop the progression of the disease. Medications play an important role in allowing you to participate fully in your physiotherapy sessions by putting your brain in the best condition to work on things such as balance, strength, and walking. You should always follow the directions of your neurologist when taking medications.
So how can physiotherapy help manage Parkinson’s Disease?
Physiotherapists are experts in pinpointing functional limitations and prescribing exercises to target these areas and restore normal movement. So, in people with Parkinson’s, this includes exercises for strength, flexibility, balance, and overall health. In fact, exercise has been shown to be the only thing that can slow the progression of Parkinson’s disease. Ultimately, physiotherapy is meant to be a complement to medication in managing Parkinson’s Disease. Below is a good resource for a Parkinson’s specific exercise program that is guided by a physiotherapist.
1. Improve balance
Balance is an important predictor of your risk of falling. People with Parkinson’s can struggle with balance because of changes in posture, strength, stiffness, and walking. In addition, people with Parkinson’s suffer from a vicious cycle of disuse where they experience limitations and as a result, lose confidence in their own ability to do certain movements. Because of this, you don’t try them as much which only worsens the problem. Physiotherapists are experts in providing balance exercises in a safe environment that are the proper challenge for you. The following are examples of exercises our physiotherapists might give you to challenge your brain and body’s ability to right itself.

2. Improve strength and flexibility
Even in normal healthy individuals, it is expected that most people will have muscle imbalances. Physiotherapists are experts in recognizing muscle limitations and prescribing exercises to target areas of weakness. For example, your physiotherapist may give you exercises to strengthen your legs to help improve your balance and walking. They can also give you exercises for your upper body to help with posture and daily activities. Lastly, they can provide you stretches or myofascial release to help manage some of the stiffness associated with Parkinson’s disease.
Quick tips for stiffness:
- Continue any exercise you enjoy within your limits
- Massage, heat, or ice can help provide some relief for stiff and sore muscles

3. Increase size of movements
People with Parkinson’s Disease often have a disconnect between what they perceive and what others around them perceive as a normal movement. LSVT BIG stands for Lee Silverman Voice Treatment which was a speech therapy created for a Parkinson’s patient. The BIG component refers to the physiotherapy program which was made based on the same principles. It is an exercise method that can be used to manage movement problems associated with Parkinson’s. Research has shown it can improve walking speed, step size, balance, and flexibility. Since Parkinson’s makes it hard to remember to use big movements this method does the opposite. Therefore, the main principle is to “think BIG” and the purpose is to retrain the muscles and relearn how normal movement should feel. At first, these movements may seem weird and feel too big. However, with practice and time, you will start to feel they are more normal.
4. Improve posture
Parkinson’s Disease affects your ability to control things that are normally automatic. For example, your posture will change without automatic reminders coming from the brain to the muscles. Did you know? With every inch forward, the weight of your head increases by 10 pounds! So you can see how this change in posture can lead to more strain on the neck and the back. Ultimately, this can lead to pain! It can also affect your breathing, loudness, and clarity when you speak. Luckily, physiotherapists can provide verbal or non-verbal cues to help slow the progression of Parkinsonian posture. As well, we can provide exercises to stretch or strengthen the postural muscles. It is important to make these changes as soon as possible. This is because spending too much time in this posture can lead to a loss of flexibility and changes in balance.
Quick tips for posture
- Use a mirror to check your posture (front and side)
- Ask a family member to remind you to change your posture if they notice you stooping
- The best position is the next position! Change positions often and take movement breaks!

5. Provide strategies to manage freezing gait and other changes
Last but not least, physiotherapists can help to provide strategies for freezing gait and festination. Freezing gait occurs when people with Parkinson’s find they are unable to take a step when they want to. This has been described as feeling like their feet have become “glued to the floor”. Meanwhile, festination is when your steps become smaller and faster. As a result, this causes your center of gravity to shift in front of your feet. Ultimately, both can lead to an increased risk for falls and injury. You may experience this when you are off your medication but it is also possible when you are on your medication. Check out these great tips to manage freezing of gait from the American Parkinson’s Disease Association!
Quick tips to manage freezing gait
Walking
- Focus on the size of each step and not the speed! Think about each step like a big kick but remember to always land your heel first.
- Come to a complete stop when you start to shuffle or freeze and RESET. Don’t fight the freeze!
- Take a breath, stand tall, and try again. Focus on taking a big step with your first step.
Turning
- Focus on lifting your feet! DO NOT pivot or spin around.
Exercise
When walking or performing your exercises it is important to:
- Stand TALL
- Shift WEIGHT
- Step BIG
- Swing BIG
Physiotherapists can help provide cues to interrupt freezing. We can also help restore normal walking patterns. As we walk, our arms and legs move at the same time but in opposite directions. For example, as you take a step with your right leg, your left arm goes forward. Try it! This is called reciprocal movement and is often lost as movements become smaller with the progression of Parkinson’s. Similarly, normal walking requires multitasking. Think about the last time you walked in a mall. Maybe you were window shopping for cheap deals or returning that ugly shirt you got as a gift. Think about how demanding it was to walk around all those people in that setting while trying to find the store you’re looking for. Physiotherapists can help manage this by using dual-task training. Essentially, this is when mental tasks are added to a motor task such as walking.

What are you waiting for?
Leave your email below and we will contact you to book a time that works for you to come in and see our Physiotherapist! If you are looking to stay in the comfort of your own home that is no problem, we can have our Physiotherapist contact you virtually or over the phone for a consultation at the earliest of your convenience. Book in with one of our physiotherapists now to help manage Parkinson’s disease!
FAQ
What is physiotherapy for Parkinson’s disease?
Physiotherapy for Parkinson’s Disease can range from strength training, gait retraining, balance training, and strategies for abnormal gait patterns.
How does physiotherapy help with Parkinson’s?
Ultimately, physiotherapy aims to help individuals with Parkinson’s stay as independent as possible for as long as possible by improving their function and quality of life. In addition, physiotherapists can help to bridge the gap between patients and doctors that have limited time and information to give.
What type of exercise is best for Parkinson’s?
The answer is it depends! While there are exercises for strength, cardio, balance, and flexibility that all individuals with Parkinson’s can benefit from, it is also important to remember that everyone will present differently. As a result, it is best to speak with a physiotherapist so they can identify your impairments and limitations and help cater exercises that are specific to you!
How does physical activity affect Parkinson’s disease?
Exercise has been shown to reduce both physical and cognitive symptoms in addition to reducing pain that individuals can present with. Additionally, exercise and physical activity have beneficial effects on things such as sleep, mood, memory as well as fatigue and depression, and secondary complications that can result from reduced mobility.

