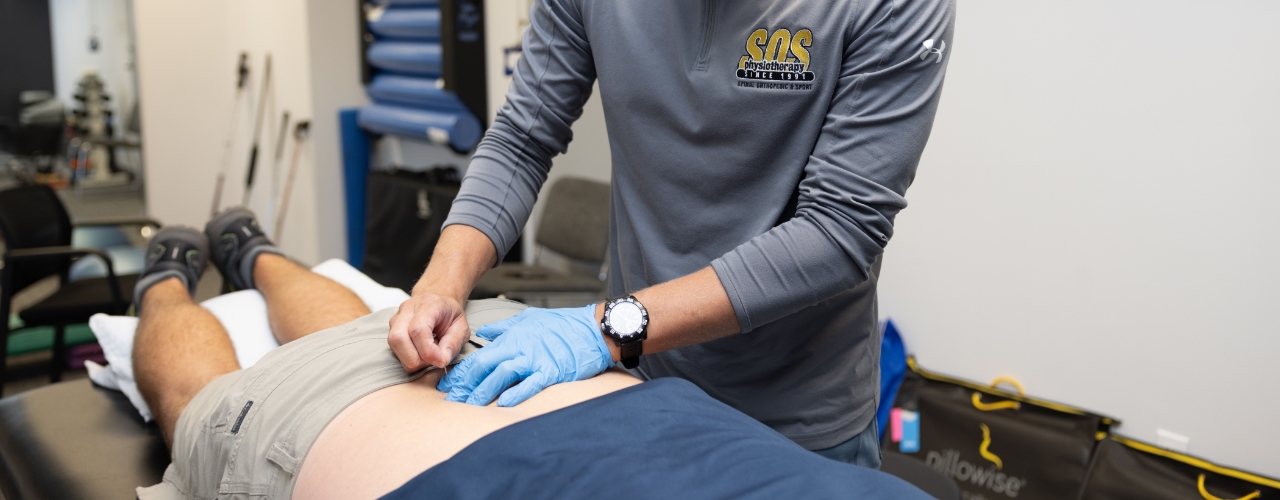
Dry needling is a treatment technique that involves the insertion of a very thin and flexible needle into a shortened muscle in order to help it relax, loosen, and function better. In most cases, multiple muscles have to be needled during a single treatment session. These painful muscles containing tight bands with tender ‘knots’ (known as trigger points) can feel ropey and are involved in many types of soft tissue pain. The trigger points are specifically targeted with the needle during treatment. The needle used is referred to as a ‘dry needle’ because there is no solution or medication being injected.
Myofascial Trigger Points
A myofascial trigger point is a hypersensitive spot, usually within a tight band of muscle or in the muscle’s fascia (surrounding tissue). (1,2) Trigger points can be tender to touch and may create pain in areas distant from the involved muscle itself, which can feel like aching, boring, and sometimes sharp pain; some myofascial trigger points cause pain without being directly provoked.(1,2)
Myofascial trigger points are associated with muscle pain, loss of flexibility and range of motion, as well as functional weakness of a muscle.(2,3)
So, how does it work?
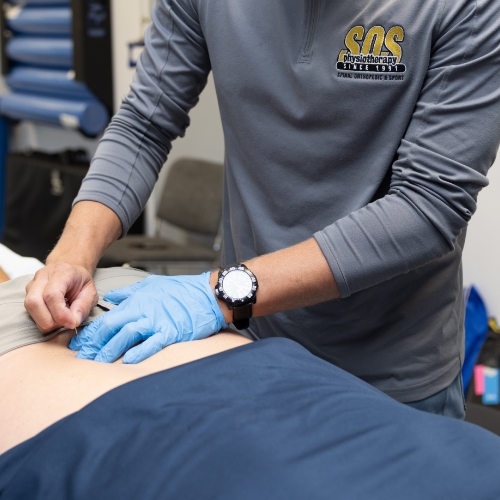
Intramuscular Stimulation (IMS) is a total system for the diagnosis and treatment of myofascial pain syndromes (chronic pain conditions that occur in the musculoskeletal system when there is no obvious sign of injury or inflammation). IMS is grounded in Western Medical Science, and has a solid foundation in its radiculopathic model of pain, which is now supported by many experts in the field. It was developed by Dr. Chan Gunn while he was a physician at the Worker’s Compensation Board of British Columbia in the 70’s, where he investigated the large number of mysteriously stubborn cases after frustration with the ineffective modalities at his disposal. The treatment, which utilizes acupuncture needles because they are the thinnest implements available that are designed to penetrate deep within muscle tissue, specifically targets injured muscles that have contracted and become shortened from distress.
IMS relies heavily on a thorough physical examination of the patient by a competent practitioner, trained to recognize the physical signs of neuropathic pain. This physical examination is indispensable since chronic pain is often neurological as opposed to structural, and therefore, invisible to expensive X-rays, MRI Tests, Bone and CT Scans. Failure to recognize these signs will result in an inaccurate diagnosis, and thus, a poor starting point for physical therapy.
The treatment involves dry needling of affected areas of the body without injecting any substance. The needle sites can be at the epicenter of taut, tender muscle bands, or they can be near the spine where the nerve root may have become irritated and supersensitive. Penetration of a normal muscle is painless; however, a shortened, supersensitive muscle will ‘grasp’ the needle in what can be described as a cramping sensation. The result is threefold. One, a stretch receptor in the muscle is stimulated, producing a reflex relaxation (lengthening). Two, the needle also causes a small injury that draws blood to the area, initiating the natural healing process. Three, the treatment creates an electrical potential in the muscle to make the nerve function normally again. The needle used in IMS, by stimulating muscle spindles, essentially becomes a specific and unique tool for the diagnosis of Neuropathic Muscle Pain.
The goal of treatment is to release muscle shortening, which presses on and irritates the nerve. Supersensitive areas can be desensitized, and the persistent pull of shortened muscles can be released. IMS is very effective for releasing shortened muscles under contracture, thereby causing mechanical pain from muscle pull. IMS, in effect, treats the underlying neuropathic condition that causes the pain. When competently performed, IMS has a remarkable success rate, as proven by the amelioration of symptoms and signs, even for chronic back pain with root signs.
This treatment method is used by our licensed Kitchener, Elmira, and Northfield, ON physiotherapists as a way to relieve pain. When performing dry needling, our physiotherapist will insert a sterile needle through the skin, into the underlying tendons, ligaments, or muscles that have been affected, in order to relieve pain, decrease muscle tension, and improve mobility.
While it is a common misconception, dry needling is not acupuncture. It is based on a modern scientific study of musculoskeletal and neuromuscular systems. While there are some similarities, dry needling is strictly based on Western medicine principles and research. It provides an environment that enhances the body’s ability to heal, ultimately reducing pain in the process.
Will dry needling hurt me?
Your Next Steps…
Request An Appointment
Receive A Custom Treatment Plan
Work Hard and Progress In Your Recovery
Recover & Enjoy Life Pain-Free!